Diagnosis
The evaluation of fainting begins with a careful medical history. In many cases, the history alone provides the most important clues. Patients are asked what they were doing at the time of the episode, whether warning symptoms were present, how long the episode lasted, and how they felt afterward. Doctors rely heavily on the history, obtained from the patient and witnesses, to help determine the most likely cause of syncope.
A physical examination follows, including careful measurement of blood pressure (which should be measured lying, sitting and standing), and any potential cardiac causes for syncope should be investigated. Changes in blood pressure with position can suggest orthostatic hypotension or other autonomic causes.
Not every patient requires extensive testing. The goal is to identify those at higher risk for cardiac causes, which may require more urgent evaluation and treatment.
In many individuals, especially younger patients with typical warning symptoms and a normal heart evaluation, the cause is reflex (vasovagal) syncope — a benign but sometimes recurrent condition.
Selected patients may undergo specific testing as follows:
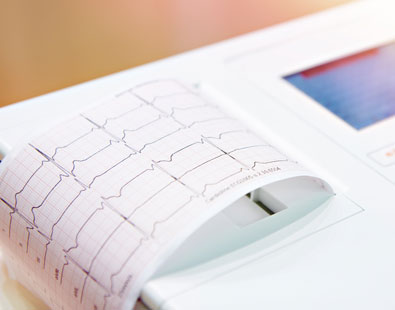
ECG. The Electrocardiogram is the most basic cardiac test. It provides valuable information about the health of the heart. It can show evidence of heart muscle abnormalities or damage. The ECG can also provide evidence of electrical disease of the heart or rhythm problems as a likely cause of syncope.
Heart Monitors. Recording the ECG during a symptom such as dizziness or fainting can provide the diagnosis in the event of a heart arrhythmia. One type of monitor is known as a “Holter Monitor” and records continuously for up to 7 days. Another type of monitor is referred to as an Event Monitor or a "Loop" recorder. Generally, these monitors automatically detect abnormal rhythms and can also record when the wearer presses a button. These monitors are able to automatically transmit recordings directly using cell phone technology. The latest technology is known as "Mobile Cardiac Outpatient Telemetry" or MCOT. The wearer is continuously connected via cell phone to the monitoring company, and the company has the ability to immediately notify the physician of any changes in the heart rhythm.
Echocardiogram. An echocardiogram is a test that uses sound waves to get a moving picture of the beating heart. We can measure the size of the heart chambers, examine the function of the heart valves, and determine if there is evidence of a prior heart attack or other abnormalities of the heart muscle. Fainting that occurs in the setting of heart disease may be due to dangerous arrhythmias, so the echocardiogram is an important test that helps the doctor to decide what to do next.
Stress Test. This is also called an exercise tolerance test, and is usually performed by having the patient walk on a treadmill while they are attached to an ECG machine. ECG changes that occur with exercise might indicate a significant coronary blockage. A “nuclear” stress test uses a radioactive tracer to get an actual picture of the blood flow to the heart muscle. Stress tests are most useful when a person fainted during or after exercise, or when the faint was associated with chest pain. Stress tests are done to rule out exercise-induced arrhythmias or coronary artery disease.
Tilt Table Test. A tilt table test should be called a standing test. The patient is placed on a horizontal table and then is tilted into an upright position, generally to an angle of 60-70 degrees, so that they are upright. The table (and the patient) remain in that position while the blood pressure and heart rate are monitored over 30-60 minutes. Sometimes medications are given to test the normal autonomic reflexes that control the heart and blood vessels. This test is primarily done to try to reproduce neurocardiogenic ("reflex" or vasovagal) syncope, or to evaluate for orthostatic hypotension or POTS.

Implantable Cardiac Monitor. If fainting occurs repeatedly and no obvious cause can be identified, a small heart monitor can be inserted under the skin. This device, also known as an Implantable Loop Recorder (ILR), is able to automatically detect and record arrhythmias. Patients can also activate it manually if they have a significant symptom. The recordings can be retrieved using a computer or even the patient's cell phone. Heart rhythm problems can be treated appropriately once the diagnosis is made. An example of an implantable cardiac monitor is shown below.
Electrophysiology (EP) Study. The EP Study is a test that is commonly done to evaluate patients for possible arrhythmias. It is relatively safe test, performed by inserting thin wire catheters into a vein to test the electrical system of the heart. It is designed to reproduce heart rhythm problems that may be causing syncope. It is usually recommended to patients with a history of underlying heart disease, or if an excessively slow or fast heart rhythm problem is suspected. Certain rapid arrhythmias like PSVT and atrial flutter can be cured permanently during the EP Study with a procedure known as Catheter Ablation.
Less useful tests that are may be ordered include brain imaging studies like a CT Scan (which uses x-rays) or MRI (which uses radio waves in a magnetic field) to detect physical abnormalities like a stroke or a brain tumor. A Carotid Ultrasound is a sound wave test to detect blockages in the neck arteries. These blockages can cause symptoms of a stroke such as weakness or numbness of part of the body, though they generally do not cause fainting. An EEG (electroencephalogram) is a recording of the brain waves. It is helpful to perform an EEG when there is a suspicion of a seizure disorder (epilepsy). It is now accepted that these tests are not particularly helpful unless the patient has other signs or symptoms of a neurological condition (like headaches, visual problems, weakness, etc.).
